What is Lyme disease?
Lyme* Disease, also known Lyme Borreliosis – is an infectious disease caused by bacteria of Borrelia type and which is spread by infected ticks genus Ixodes. Borrelia belongs to the spirochaeta bacteria type: Borrelia burgdorferi, Borrelia garinii, Borrelia afzelii, Borrelia japonica. The tick becomes infected after feeding on infected deer or mice. Humans get infected through saliva or vomited matter by a blacklegged tick. The natural reservoir of spirochaete are several animal species, rodents mainly.
*Lyme - and more proprely Old Lyme – it is a town in Connecticut, in the USA, where Lyme Borreliosis has been diagnosed as separate disease entity in 1975 for the first time.
Four stages of Lyme disease
- Stage 1 – an early early localized Lyme disease, and may last for 1 to 4 weeks.
- Stage 2 – an early disseminated Lyme disease.
- Stage 3 – a late disseminated Lyme disease.
- Stage 4 – a chronic Lyme disease, so called arthritic.
The stages 3 and 4 of Lyme disease should be taken into consideration when differentiating. This may happen when an early stage has not been noticed or was miss diagnosed.
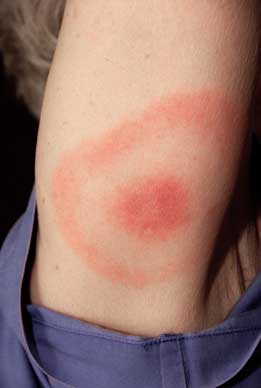
Early Lyme disease symptoms include flu-like illness (fever, chills, sweats, muscle aches, fatigue, nausea and joint pain) and very characteristic skin rash so called erythema migrans. This is the most common early symptom of Lyme disease (approx. 70 % of cases). In some patients borrelia infection may be associated with lymphocytic infiltrate of the skin. Lymphocytic skin infiltrate described by Jessner and Kanof in 1953, is a skin condition characterized by small, red, bumps on the face, neck, and upper back. The bumps usually last for several months or longer and can enlarge to create a red plaque. Typically, there are no other symptoms, although rarely, individuals may experience burning or itching. The symptoms may fluctuate between periods of worsening and periods of improvement. To see the pictures and to read more → Jessner lymphocitic skin infiltrate.
The cause of Jessner lymphocytic infiltrate is unknown. It is classified as a benign T-cell lymphoproliferative disorder. Some cases have been associated with borrelia infection, the cause of Lyme disease.
The early symptoms retreat within 3 months and an early disseminated stage develops in part of the patients.
Diagnosis
Lyme disease diagnosis comprise of several tests that each has its own specificity. We receive test result from laboratory and go to see a doctor who renders received result. The essential parameter is so called reference norm. We may hear: result is in the normal range or is above or is below the norm. If the test was made for specific bacteria, fungus or virus result should determine whether we have specific infection (positive result or negative results). However, one has to underline that Lyme disease affects immune system so approx. 20 – 30 % of patients has false negative test for borrelia spirochaeta antibodies.
Negative result of ELISA test (enzyme-linked immunosorbent assay) (particularly in advanced stage of Lyme disease) does not exclude Lyme disease.
Diagnostic Tests
The Centers for Disease Control and Prevention (CDC) currently recommends a two-tiered testing approach: a conventional enzyme-linked immunoassay (ELISA) test, followed by a Western Blot test. The ELISA is a blood test that detects antibodies but does not test for B. burgdorferi itself. A positive result from this first-level screening may suggest current or past infection. The ELISA is designed to be very “sensitive,” meaning that almost everyone who has Lyme disease (and some people who do not) will test positive. If the screening test is negative, it is highly unlikely that the person has Lyme disease and no further testing is recommended. If the screening test is positive or inconclusive, a Western blot test should be performed to confirm the results.
Used appropriately, the Western blot test is designed to be "specific", meaning that it will usually be positive only if a person has been truly infected by B. burgdorferi. If the Western blot is negative, it suggests that the ELISA test was a false positive.
CDC does not recommend testing by Western blot without first using the ELISA. Using the Western blot on its own makes a false positive result more likely. Such results may lead to people being treated for Lyme disease when they do not have it, instead of being treated for the true cause of their illness.
Other Diagnostic Tests for Lyme Disease
- LTT Assay (lymphocyte transformation test) – is an assay which allows to measure the activity of peripheral blood Th cells against specific antigens. T cell activation starts shortly after infection, with T cells proliferation and the production of cytokines (such as INF-γ) which regulate the adaptive immune response. LTT assay is popular in Europe for the diagnosis of Lyme disease, use full length OspC* of B. burgdorferi as one of their antigens and request a positive stimulation index against only one or two antigens, in order to be considered positive. In what follows, we demonstrate that, in case of patients with gut bacteria translocation, such a test has a theoretical risk of false positive results.
*OspC is a major surface protein produced by Borrelia burgdorferi when infected ticks feed but whose synthesis decreases after transmission to a mammalian host.
- Molecular biology techniques: PCR and rtPCR – Polymersae Chain Reaction and real time Polymersae Chain Reaction (more sensitive) is used to confirm tick-borne diseases e.g. Borrelia burgdorferi infection. Extension of PCR method in laboratory diagnostics of Lyme disease (LD) gives a possibility of confirmation of spirochaete infection before patient body managed to produce antibodies. Diversity of material, which may be tested (blood, cerebrospinal fluid, skin biopsies, synovial fluid) and possibility of using several conservative genes for Borrelia genospecies additionally widen a diagnostic utility of PCR tests. On the other hand PCR test detects DNA (genetic material) of spirochaeta in the sample obtained from patient (blood, cerebrospinal fluid, skin biopsies, synovial fluid, etc.) not in the body. However, it may happen, in the late phase of Lyme disease when spirochaeta have setteld in various internal organs and/or connective tissue, that the sample does not contain spirochaeta genetic material. And due to that fact PCR test may show false negative result. The sensitivity could be enhanced by administration of antibiotics or chemotherapeutics that could induce spirochaeta release from organs and tissues into blood stream.
- LUAT Test – Lyme Urine Antigen Test (spirochaeta antigens in urine) – 30% of Lyme disease patients had a positive LUAT test. The antibiotic therapy may induce antigenuria (so called: antibiotic challange ) multiple testing might be helpful in therapy mornitorning (efficacy control).
Lyme disease become so universal and frequent problem that several organisations have been created to support research and treatment and also to organize people involved in whole subject. One of such organizations is Global Lyme Alliance in Stamford, Connecticut and not very fare from Old Lyme town where disease has been described firstly. Click the link to visit their web site.