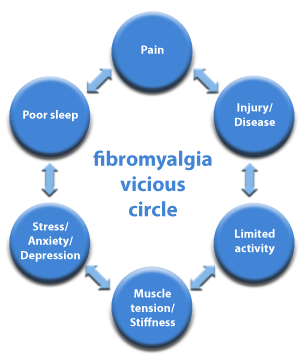
Fibromyalgia syndrome comes with large variety of symptoms. Symptoms of fibromyalgia come in many shapes and sizes and their intensities is related to various exogenous/extrinsic and endogenous/intrinsic stress factors just to mention some of them: injury, cold, humidity, infection, psycho-social factors. The variety and relatively low specificity of symptoms makes that fibromyalgia is often confused with other conditions and its diagnosis is difficult. One has to underline that fibromyalgia is non-inflammatory illness and due to this fact there are not present clinical symptoms of inflammation* neither are present lab results typical for inflammation.
Pain Symptoms
Chronic Widespread Pain
Fibromyalgia has many symptoms that tend to vary from person to person. The main symptom is widespread pain.
There may be periods when your symptoms get better or worse, depending on factors such as:
- your stress levels
- changes in the weather
- how physically active you are
If you think you have fibromyalgia, visit your GP. Treatment is available to ease some of the symptoms, although it's unlikely they'll ever disappear completely.
The main symptoms of fibromyalgia are outlined below.
Widespread pain
If you have fibromyalgia, one of the main symptoms is likely to be widespread pain. This may be felt throughout your body, but could be worse in particular areas, such as your back or neck. The pain is likely to be continuous, although it may be better or more severe at different times.
The pain could feel like:
- an ache
- a burning sensation
- a sharp, stabbing pain
Pain is the main and dominating symptom of fibromialgia. The pain is chronic – lasts longer than 3 months and it is disseminated (widespread) that means affects at least three from all four body quadrants. The pain has wavy character with intervals of exacerbation and mellowing. Patients may very suggestively and dramatically describe their pain:
- Dull, deep aching pain
- Sharp, stabbing pain
- Radiating or shooting pain
- Stinging pain that feel like a sunburn or pins and needles
- Strange sensations that feel like crawling, tingling, burning, itching or numbness
- Shocking pain, it can feel like electricity zinging along the nerve and explodes in a certain area
Keeping a pain diary is a good way to track your pain over time and will help you be more specific at your doctor appointments. You can also use the American Pain Foundation’s L O C A T E S memory aid. It is a good way to remember how to describe your pain. Each letter of L O C A T E S stands for information you should tell your doctor:
L – Location of the pain and whether it travels to other body parts.
O – Other associated symptoms such as nausea, numbness, or weakness.
C – Character of the pain, whether it’s throbbing, sharp, dull, or burning.
A – Aggravating and alleviating factors. What makes the pain better or worse?
T – Timing of the pain, how long it lasts, is it constant or intermittent?
E – Environment where the pain occurs, for example, while working or at home.
S – Severity of the pain. Use a 0-to-10 pain scale from no pain to worst ever.
Physical activity induces (amplifies) fibromyalgia pain and this, together with chronic fatigue, leads to the characteristic fibromyalgia feature – so called exercise intolerance.
Characteristic Pain Location
Pain in fibromyalgia most often affects periarticular (joint surrounding) tissues: muscle tendons, muscle origins (bone attachments), ligaments, fascias, and joint surrounding structures (synovial bursae, tendons’ sheaths). Due to such localization it often mistaken as join pain but it is not. Joints normally are not affected in fibromyalgia. However, if pain and stiffness last for pretty long time it may lead to joint changes in years.
Characteristic pain locations can be found by looking at the location of → tender points. The current diagnostic criteria (established in 2010) are based on number of specific areas in which patient experiences pain. The list covers 9 pairs of bilateral sites corresponding to the previous (tender points) and new unilateral (axial) sites: neck, chest, abdomen, upper back, lower back and new bilateral site: jaw.
Exceptional Sensitivity to the Pain Stimuli
People suffering from fibromyalgia reveal exceptional whole body sensitivity (vulnerability) to different stimuli, so even the lightest touch may cause pain. If you e.g. broke your nail – the pain will be much stronger and last much longer than normally.
This phenomenon is deffined as:
- Hyperalgesia – is an increased sensitivity to pain, which may be caused by damage to nociceptors** or peripheral nerves. Prostaglandins E and F are largely responsible for sensitizing the nociceptors. Temporary increased sensitivity to pain also occurs as part of sickness behaviour, the evolved response to infection.
- Allodynia – is a pain resulting from a stimulus (such as a light touch of the skin) which would not normally provoke pain. Allodynia results to central pain sensitization (increased response of neurons). Allodynia can lead to the triggering of a pain response from stimuli which do not normally provoke pain. Temperature or physical stimuli can provoke allodynia, which may feel like a burning sensation.
Note: hyperalgesia – exaggerated reaction to pain stimuli, allodynia – pain reaction to non-pain stimuli.
Moreover, fibromyalgia patient may show exaggerated reaction to various stimuli and situations like for example smoke, some food, bright light, some sounds. Exposition to such stimuli may trigger or exaggerate other fibromyalgia symptoms.
Muscle Stiffness
Fibromyalgia is known to cause muscle pain which can contribute towards muscle stiffness. Stiffness in the joints or muscles can restrict our mobility, having a debilitating impact on our day to day lives.
Stiffness of muscles and joints is the feeling that a joint will not easily move and does not feel comfortable. It is often accompanied by pain, and it can be hard to bear weight on the affected joint. For fibromyalgia sufferers, the stiffness is often worse in the morning, making it difficult to get going and ready for the day ahead. This can have a negative effect every day activity.
As muscle pain is a primary symptom of fibromyalgia, this may contribute to muscle stiffness. Generally when a joint feels sore, you will be reluctant to move it. However, this can mean that you lose elasticity and flexibility in the joint, causing it to progressively become stiffer. During the night, we do not use or move our limbs as much as during the day, which may explain why stiffness is often worse in the morning.
Additionally, some studies suggest that the arteries of fibromyalgia patients, which should be flexible and strong, are often weaker and less efficient. This leads to poor circulation and a less efficient blood supply to muscle and joints, another possible contributor to stiffness.
Mental and Cognitive Symptoms
Mental and cognitive symptoms are commonly accompanying fibromyalgia. Just to mention to most frequent:
- Sleep disorders – in approx. 70 % patients
- Cognitive, memory, concentration and coordination problems – in approx. 50 – 70 % patients
- Low mood and depression – in more than 60 % patients
- Fear and anxiety – in approx. 56 % patients
According to different sources 20 – 70 % of fibromyalgia patients manifest psychopathological symptoms like anxiety state, nervous tension, personality disorder, psychasthenia†, dissociative disorder‡, or depression. Their revelation depends on genetic propensity. It is believed that they belong along with vegetative and functional symptoms to integral clinical picture of fibromyalgia. Fibromyalgia is sometimes wrongly perceived as a "pain mask" of depression. This question is presented in bookmark → Fibromyalgia or Depression
______________________
*Inflammation is characterized by five cardinal signs: rubor (redness), calor (increased heat), tumor (swelling), dolor (pain), and functio laesa (loss of function). The first four signs were first established by Aulus Cornelius Celsus in his work De Medicina (1st Century BC), and are known by the name Celsus tetrad. The fifth sign – functio laesa – was given by Aelius Galenus, a Greek physician, surgeon and philosopher in the Roman Empire 2nd/3rd century AD.
**A nociceptor is a sensory neuron that responds to damaging or potentially damaging stimuli by sending “possible threat” signals to the spinal cord and the brain. If the brain thinks the threat is credible, it creates the sensation of pain to direct attention to the body part, so the threat can hopefully be mediated. This process is called nociception.
†Psychasthenia is a psychological disorder characterized by phobias, obsessions, compulsions, or excessive anxiety
‡Dissociative disorders (DD) are conditions that involve disruptions or breakdowns of memory, awareness, identity, or perception. People with dissociative disorders use dissociation, as a defence mechanism, pathologically and involuntarily. Some dissociative disorders are triggered by psychological trauma, but dissociative disorders such as depersonalization/derealization disorder may be preceded only by stress, psychoactive substances, or no identifiable trigger at all.